Posterior Fossa Epidural Hematoma: A Case Report
DOI:
https://doi.org/10.46900/apn.v8i2.2026Keywords:
Pediatric Neurosurgery, Epidural hematoma, Posterior FossaAbstract
Introduction/Background:
Posterior fossa epidural hematoma (PFEDH) is a rare entity within pediatric traumatic brain injury, characterized by blood accumulation between the dura mater and skull in the infratentorial compartment. Despite its low incidence, PFEDH carries significant risk due to the limited compliance of the posterior fossa, which may lead to brainstem compression, hydrocephalus, and rapid neurological deterioration. Clinical presentation is often subtle and nonspecific, contributing to delayed diagnosis and increased morbidity.
Case Presentation:
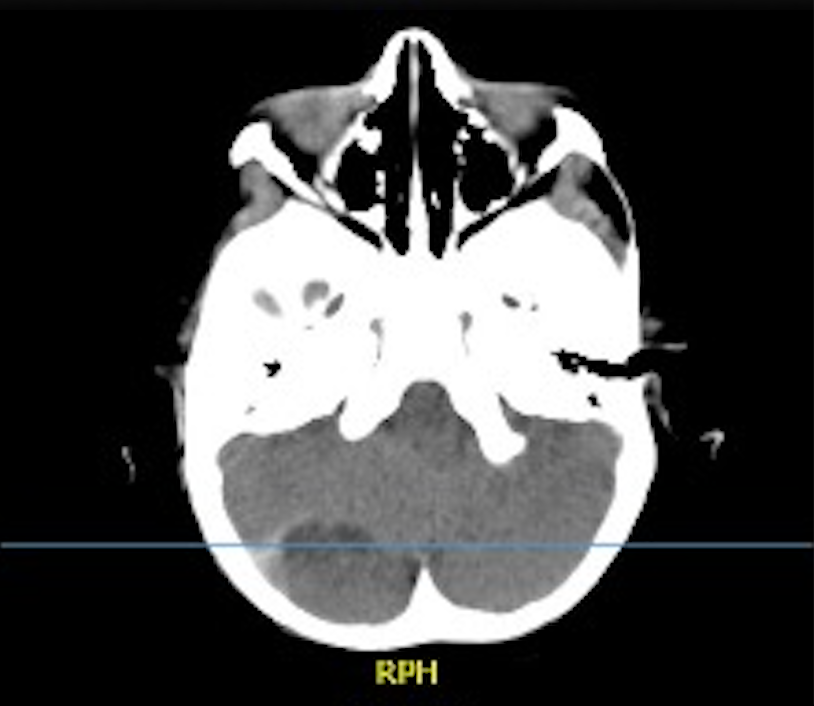
A previously healthy 4-year-old girl presented with persistent vomiting following occipital head trauma after a fall. Initial evaluations misdiagnosed the condition as gastroenteritis, delaying neuroimaging. Progressive symptoms, including drowsiness and prostration, prompted cranial computed tomography, which revealed a posterior fossa epidural hematoma (4.3 × 3.0 × 1.8 cm) associated with ventriculomegaly and signs of intracranial hypertension. Despite a Glasgow Coma Scale score of 15 and absence of focal deficits, surgical intervention was indicated due to mass effect and cerebrospinal fluid obstruction. The patient underwent occipital craniotomy with hematoma evacuation. The postoperative course was uneventful, with rapid clinical improvement and complete recovery at follow-up.
Conclusions:
PFEDH may present with nonspecific symptoms in pediatric patients, increasing the risk of diagnostic delay. This case highlights the importance of maintaining a high index of suspicion and early use of neuroimaging in children with persistent vomiting after head trauma. Prompt surgical management, even in neurologically stable patients, can lead to excellent outcomes and prevent severe complications.
Downloads
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Lucas Rodrigues Olmedo, Álvaro Kalil Abrahão Fiumari, Otávio da Cunha Ferreira Neto, Ruan Krubniki Ferraz, Stephanie Naomi Funo de Souza, Ricardo dos Santos Oliveira

This work is licensed under a Creative Commons Attribution 4.0 International License.

When publishing in Archives of Pediatric Neurosurgery journal, authors retain the copyright of their article and agree to license their work using a Creative Commons Attribution 4.0 International Public License (CC BY 4.0), thereby accepting the terms and conditions of this license (https://creativecommons.org/licenses/by/4.0/legalcode).
The CC BY 4.0 license terms applies to both readers and the publisher and allows them to: share (copy and redistribute in any medium or format) and adapt (remix, transform, and build upon) the article for any purpose, even commercially, provided that appropriate credit is given to the authors and the journal in which the article was published.
Authors grant Archives of Pediatric Neurosurgery the right to first publish the article and identify itself as the original publisher. Under the terms of the CC BY 4.0 license, authors allow the journal to distribute the article in third party databases, as long as its original authors and citation details are identified.





























